Virtual Clinicals: Enhancing Nursing Education through Technology

Table of Contents
Name of the heading 1
1- Start your table with the syntax {start-table}
2 - Add an H3 Heading to create a new column (this will be the column title)
3 - List cells as bullet points in a List element
4 - End your table with the syntax {end-table}
Nursing education plays a vital role in preparing future healthcare professionals for the complex challenges of patient care. Traditionally, nursing students have relied on clinical rotations to gain hands-on experience and develop critical skills. However, the advancement of technology has introduced innovative solutions that are revolutionizing nursing education. One such solution is the integration of virtual clinicals, which leverage immersive technology to enhance the learning experience for aspiring nurses.
In this article, we explore research on the role of simulation in virtual clinicals and the benefits and potential of virtual clinicals in nursing education, highlighting how this technology can shape the future of healthcare training.
Research on the role of simulation in virtual clinicals
A landmark study by Hayden et al. (2014) conducted under the auspices of the National Council State Board of Nursing (NCSBN) provides significant guidance for nursing schools regarding the substitution of traditional clinical experiences with simulation-based learning. The study, which spanned 10 different nursing schools, evaluated the potential of integrating simulation across various aspects of the nursing curriculum, including fundamentals, medical-surgical, advanced medical-surgical, maternal-newborn, pediatrics, mental health, and community health.
The findings of this comprehensive study were that up to 50% of traditional clinical experience can be effectively replaced with simulation in all core courses throughout the pre-licensure curriculum. Importantly, the study also found that NCLEX pass rates were unaffected by the substitution of real clinical experience with simulation.
In light of these findings, the NCSBN proposed key recommendations for pre-licensure nursing programs (Alexander et al, 2015). This guidance underscores the growing recognition of simulation-based learning as a viable, effective, and potentially transformative approach in nursing education.
UbiSim is the world’s first immersive VR training platform for nursing students. Learn more.
How virtual clinicals benefit nursing education
1. Simulating real-world scenarios
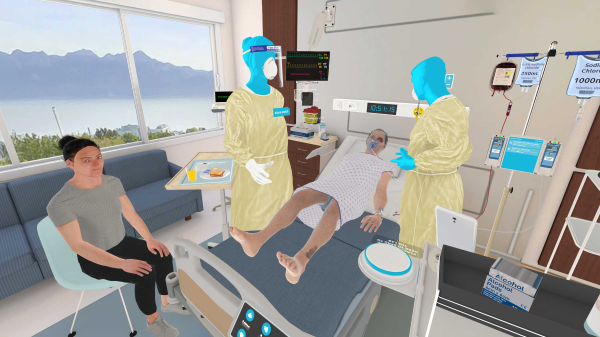
Virtual clinicals enable nursing students to engage in realistic, simulated healthcare environments. These immersive experiences mimic real-world scenarios, allowing students to practice critical thinking, decision-making, and clinical skills in a safe and controlled setting. Through virtual clinicals, students can encounter a wide range of patient cases, from routine to complex, enhancing their clinical judgment and problem-solving abilities.
Professor Tina Barbour-Taylor, Ph.D., MSN, RN from the University of West Florida, said about using UbiSim with her students, “The students really feel like they’re in the environment where the patient is. I even had a student yesterday who was trying to bump the med cart with her hip to close the drawer. And I got so tickled by that! It really felt real for her.”
Request the full case study on UbiSim’s site.
2. Accessible and flexible learning
One of the significant advantages of virtual clinicals is their accessibility and flexibility. Unlike traditional clinical rotations that are often constrained by time and availability, virtual clinicals can be accessed anytime and anywhere. Students can engage with the virtual platform from within a dedicated simulation lab or from their own homes rather than having to be in a medical setting. This flexibility allows nursing programs to accommodate a larger number of students and provides opportunities for distance learning, benefiting individuals who may have limited access to clinical placements.
3. Active learning and interactivity
Virtual clinicals foster active learning by encouraging student engagement and interactivity. These platforms often include interactive patient avatars and multimedia resources that enable students to actively participate in the learning process. Through virtual simulations, students can practice procedures, administer medications, and communicate with patients, developing essential skills while receiving immediate feedback. The ability to repeat scenarios and learn from mistakes empowers students to build confidence and competence in a supportive environment.
4. Cost-effectiveness and resource optimization
Implementing virtual clinicals in nursing education can offer significant cost savings for institutions. While traditional clinical rotations require substantial resources, including faculty supervision, transportation, and coordination with healthcare facilities, virtual clinicals eliminate many of these expenses. Additionally, virtual simulations can be scaled to accommodate large cohorts of students simultaneously, optimizing the use of resources and reducing logistical challenges.
5. Bridging the gap between theory and practice
Virtual clinicals serve as a bridge between theoretical knowledge and clinical application. Nursing students can apply the concepts they learn in the classroom directly to virtual patient care scenarios, enhancing their understanding and retention of key nursing principles. By experiencing the consequences of their decisions in a safe environment, students develop a deeper appreciation for the implications of their actions and the importance of evidence-based practice.
Barbour-Taylor from UWF said about her student’s use of UbiSim, “It builds their confidence when they go into the clinical realm to be able to say, ‘OK, so this is what I learned in the classroom, this is what I learned in simulation, now I can see how I would use that in clinical,’” she added. “For me, it’s huge to see the light bulb go off for students.”
Conclusion
Virtual clinicals have emerged as a valuable tool in nursing education, revolutionizing the way students learn and prepare for real-world healthcare challenges. By providing immersive, accessible, and interactive learning experiences, virtual clinicals enhance critical thinking, decision-making, and clinical skills among nursing students. As technology continues to evolve, the potential for virtual clinicals to become an integral part of nursing education grows. By embracing these advancements, educators and institutions can ensure that future nurses are equipped with the knowledge and skills needed to provide high-quality care in an ever-changing healthcare landscape.
Request a UbiSim demo today.
FAQs
Heading 1
Heading 2
Heading 3
Heading 4
Heading 5
Heading 6
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur.
Block quote
Ordered list
- Item 1
- Item 2
- Item 3
Unordered list
- Item A
- Item B
- Item C
Bold text
Emphasis
Superscript
Subscript
Explore more

How Immersive VR Prepares Nurses for the Demands of Real Patient Care
Discover how immersive VR simulation builds clinical judgment and confidence in nurses using a real Med-Surg scenario as the guide.
From Make-Up Hours to Mastery: VR for Clinical Judgment
Discover how VR simulation moves nursing programs from seat-time compliance to measurable clinical judgment, with evidence to back it up.
.jpg)
Preparing Practice-Ready Nurses: How the 2026 NCLEX-RN Updates Reinforce the Role of Immersive Learning
2026 NCLEX-RN updates raise the bar on clinical judgment, equity, and safety. VR simulation helps nursing programs align curriculum and close the readiness gap.


