Tech-Savvy Nursing: Using Immersive Virtual Reality to Combat Sepsis in Hospitals
.jpeg)
Table of Contents
Name of the heading 1
1- Start your table with the syntax {start-table}
2 - Add an H3 Heading to create a new column (this will be the column title)
3 - List cells as bullet points in a List element
4 - End your table with the syntax {end-table}
Did you know that sepsis is responsible for one in every three hospital deaths? Despite advances in medicine, it remains a grim reaper within our healthcare systems. Nurses, with their constant patient interaction, have the potential to be the most effective people to battle against this deadly condition. Read on to discover how immersive virtual reality can help nurses fight sepsis.
Advantages of Virtual Reality Training to Combat Sepsis
Virtual reality isn't just for gamers and tech enthusiasts anymore; it's finding a life-saving application in healthcare, particularly in the fight against sepsis.
Realistic Scenarios
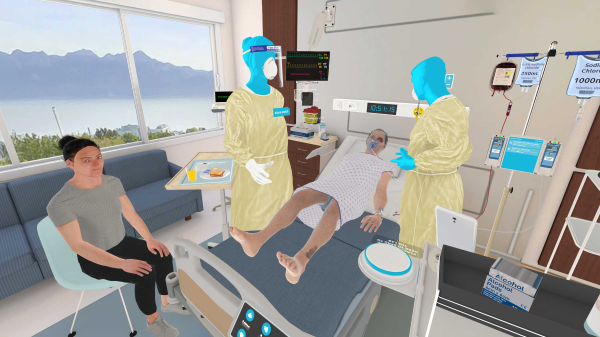
Virtual Reality (VR) allows for an extremely lifelike simulation of actual healthcare environments, complete with virtual patients displaying signs and symptoms of sepsis. This gives nurses a unique opportunity to practice identifying and treating sepsis in a controlled setting that mimics real-world conditions. Such exposure helps nurses become more adept at recognizing the signs of sepsis early when intervention is most effective.
Boston Children’s Hospital uses UbiSim, a virtual reality training platform built just for nurses. Jeff Jacobson, SIMEngineering XR Project Manager, shared“Trainees do the sepsis simulation on the manikins first then they do a VR sepsis simulation in UbiSim that we wrote ourselves. There are some things you can do in VR that you can't do in real life. You can have the virtual patient change color, talk, cough, it can do all sorts of things that a manikin just can't do.”
Emotional Preparedness
Dealing with sepsis is not just a technical challenge but an emotional one, as the stakes are often life and death. VR’s immersive environment can simulate the stress and urgency of such situations, helping nurses build emotional resilience and improving their ability to perform under pressure.
Repeated Practice
VR training allows for deliberate practice without requiring extensive resources, like patient mannequins or medical supplies. This repeated exposure helps ingrain best practices and guidelines, making them second nature for the nursing staff.
Cost-Effectiveness and Scalability
Once developed, VR modules can be reused multiple times at relatively low incremental costs, making them a cost-effective solution for ongoing training. This is especially beneficial for large healthcare institutions or systems that need to train a significant number of nursing staff. VR programs can also be updated easily to incorporate new guidelines or best practices, ensuring that the training material remains current and applicable.
Feedback
VR training modules often come with feedback mechanisms that offer evaluations, pointers, and performance analytics. This feedback allows nurses to correct mistakes immediately, solidifying proper technique and decision-making processes more effectively than traditional training could.
After each session in UbiSim, the learner will see automatically generated results/feedback. This includes all the actions they took during a session and identifies critical actions they successfully performed and performance gaps (critical actions they missed or actions they performed which they really should not have e.g., giving a patient the wrong medication).
Conclusion
Immersive Virtual Reality is proving to be more than just a technological novelty; it's a potent tool in the battle against sepsis. By offering an immersive, interactive, and emotionally charged training environment, VR helps prepare nurses for the real-world challenges they will face in their roles as primary caregivers. As hospitals look to reduce sepsis-related deaths, incorporating VR into their training programs could be a step in the right direction, bridging the gap between traditional learning and real-world application.
FAQs
Heading 1
Heading 2
Heading 3
Heading 4
Heading 5
Heading 6
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur.
Block quote
Ordered list
- Item 1
- Item 2
- Item 3
Unordered list
- Item A
- Item B
- Item C
Bold text
Emphasis
Superscript
Subscript
Explore more

How Immersive VR Prepares Nurses for the Demands of Real Patient Care
Discover how immersive VR simulation builds clinical judgment and confidence in nurses using a real Med-Surg scenario as the guide.
From Make-Up Hours to Mastery: VR for Clinical Judgment
Discover how VR simulation moves nursing programs from seat-time compliance to measurable clinical judgment, with evidence to back it up.
.jpg)
Preparing Practice-Ready Nurses: How the 2026 NCLEX-RN Updates Reinforce the Role of Immersive Learning
2026 NCLEX-RN updates raise the bar on clinical judgment, equity, and safety. VR simulation helps nursing programs align curriculum and close the readiness gap.


