
Table of Contents
Name of the heading 1
1- Start your table with the syntax {start-table}
2 - Add an H3 Heading to create a new column (this will be the column title)
3 - List cells as bullet points in a List element
4 - End your table with the syntax {end-table}
Clinical Judgment: NCSBN Model and its Role in Nursing Education
Nurses often must make split-second decisions about a patient, drawing from their experience and knowledge. How exactly are these decisions made? With clinical judgment.
Strong clinical judgment skills are crucial for patient safety. In fact, studies have shown that up to 65% of adverse events in hospitals result from poor clinical decision-making and could have been prevented.
Unfortunately, many novice nurses do not have adequate clinical judgment skills. Another study examined newly graduated nurses and found that an average of only 9% scored in the acceptable competency range for a novice nurse.
If you’re a nursing student, you’re going to have to understand the NCSBN Clinical Judgment Measurement Model (NCJMM). The Next Gen NCLEX is based on this model, and implementing the model in your nursing practice is crucial to clinical success.
So, what exactly is the NCJMM?
What is the NCSBN Clinical Judgment Model?
The NCSBN Clinical Judgment Measurement Model is a critical component of the Next Gen NCLEX and a part of how nurses succeed in their professions. It has six steps. According to the Next Gen NCLEX site, it’s “a framework for the valid measurement of clinical judgment and decision making within the context of a standardized, high-stakes examination.”
Here’s a graphic that shows the layers of this model:

What Are the Six Skills in the Clinical Judgment Measurement Model?
- Recognize cues: Nursing professionals must possess the skill to identify relevant cues or pieces of information that are essential in the assessment phase. The recognition of cues allows nurses to gather data and gain a comprehensive understanding of the patient's condition, which is vital for making accurate clinical judgments.
- Analyze cues: Once the relevant cues have been identified, nurses must have the competency to analyze and interpret these cues effectively. This involves critically thinking about the data collected, looking for patterns or connections, and drawing logical conclusions. By analyzing cues, nurses can identify potential issues or outcomes and develop appropriate interventions.
- Prioritize hypotheses: Nurses must be able to prioritize the potential hypotheses or explanations for the patient's condition based on the cues and data analyzed. This skill helps in narrowing down the possible diagnoses and treatment options, ensuring that the most crucial issues are addressed promptly and effectively.
- Generate solutions: This involves coming up with potential interventions or actions that will address the identified issues and contribute to positive patient outcomes. Nurses need to think critically and creatively to generate suitable solutions that are evidence-based and align with best practices in nursing care.
- Take action: Nurses must have the competency to execute the planned interventions in a timely and effective manner. This involves collaborating with the healthcare team, coordinating resources, and providing patient-centered care. Taking action requires not only clinical expertise but also effective communication and organizational skills.
- Evaluate outcomes: Once the interventions have been implemented, nurses must assess the effectiveness of the actions taken and their impact on the patient's condition. This skill involves monitoring the patient's progress, assessing the attainment of desired outcomes, and making necessary adjustments to the plan of care as needed. Evaluation helps nurses gauge the success of their clinical judgments and identify areas for improvement.
What was the impact of the NCJMM on the NCLEX?
The impact of the NCJMM on the Next Gen NCLEX, the nursing licensure and certification exam, has been transformative. The NCJMM, developed by the National Council of State Boards of Nursing (NCSBN), revolutionized the way clinical judgment is measured in the nursing field.
Before the implementation of the NCJMM, the NCLEX primarily focused on testing knowledge and recall of facts, with less emphasis on the critical thinking and decision-making skills that are crucial for effective nursing practice. However, with the introduction of this innovative measurement model, the Next Gen NCLEX now evaluates a nurse candidate's ability to apply clinical judgment in real-world scenarios.
By incorporating the NCJMM into the NCLEX, the NCSBN has ensured that aspiring nurses are not only competent in their knowledge base but also proficient in clinical reasoning and judgment. This shift in focus reflects the evolving demands of the nursing profession, where nurses are expected to be highly skilled in critical thinking and problem-solving.
The NCJMM has not only influenced the way the NCLEX is designed but has also had a broader impact on nursing education and practice. Nursing programs have been prompted to align their curricula with the NCJMM framework, integrating opportunities for students to develop and refine their clinical judgment skills. This has led to a more comprehensive and holistic approach to nursing education, emphasizing the importance of critical thinking and clinical reasoning throughout the learning process.
Furthermore, the NCJMM has provided a standardized language and framework for nursing educators and practitioners to discuss and evaluate clinical judgment. It has become a valuable tool in nursing research and the development of evidence-based practices. The measurement model has facilitated collaboration among educators, researchers, and regulators, fostering a shared understanding of clinical judgment and its assessment.
Final Thoughts
In conclusion, the NCJMM is a critical framework for measuring clinical judgment and decision-making skills in nursing. It consists of six key skills: recognizing cues, analyzing cues, prioritizing hypotheses, generating solutions, taking action, and evaluating outcomes. The NCJMM plays a crucial role in ensuring that nursing professionals possess the necessary skills for safe and effective patient care.
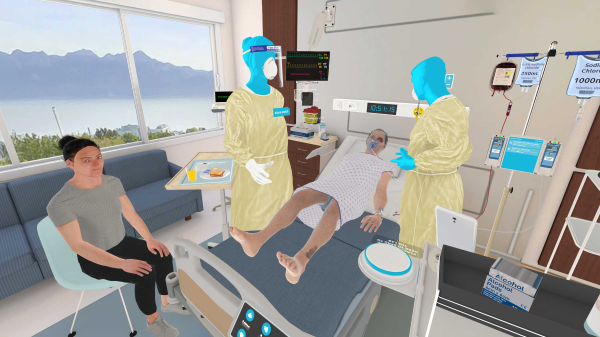
One way to train nursing students to develop clinical judgment is with virtual reality simulation. UbiSim offers a cutting-edge platform built just for nursing. Request a demo today.
FAQs
Heading 1
Heading 2
Heading 3
Heading 4
Heading 5
Heading 6
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur.
Block quote
Ordered list
- Item 1
- Item 2
- Item 3
Unordered list
- Item A
- Item B
- Item C
Bold text
Emphasis
Superscript
Subscript
Explore more

How Immersive VR Prepares Nurses for the Demands of Real Patient Care
Discover how immersive VR simulation builds clinical judgment and confidence in nurses using a real Med-Surg scenario as the guide.
From Make-Up Hours to Mastery: VR for Clinical Judgment
Discover how VR simulation moves nursing programs from seat-time compliance to measurable clinical judgment, with evidence to back it up.
.jpg)
Preparing Practice-Ready Nurses: How the 2026 NCLEX-RN Updates Reinforce the Role of Immersive Learning
2026 NCLEX-RN updates raise the bar on clinical judgment, equity, and safety. VR simulation helps nursing programs align curriculum and close the readiness gap.


